The patient only lacks capacity if the answer to both questions is YES:
Does the patient have impairment/disturbance of brain function?
If YES, does this mean they are unable to make a decision as a result?
To assess ability to make a decision, you must determine if the patient can:
If the patient can still do all of these, then the patient has capacity.
If a patient over 18 years old lacks capacity, it is the doctor’s duty to make the decision on their behalf, acting in their best interests under the Mental Capacity Act. The relatives/friends have no legal right to make the decision unless they have power of attorney (for health and welfare). To decide upon the patient’s best interests, you must:
NB: if a life-changing decision needs to be made for a patient who lacks capacity and does not have relatives who can be involved, an opinion from an independent mental capacity advocate (IMCA) should be requested.
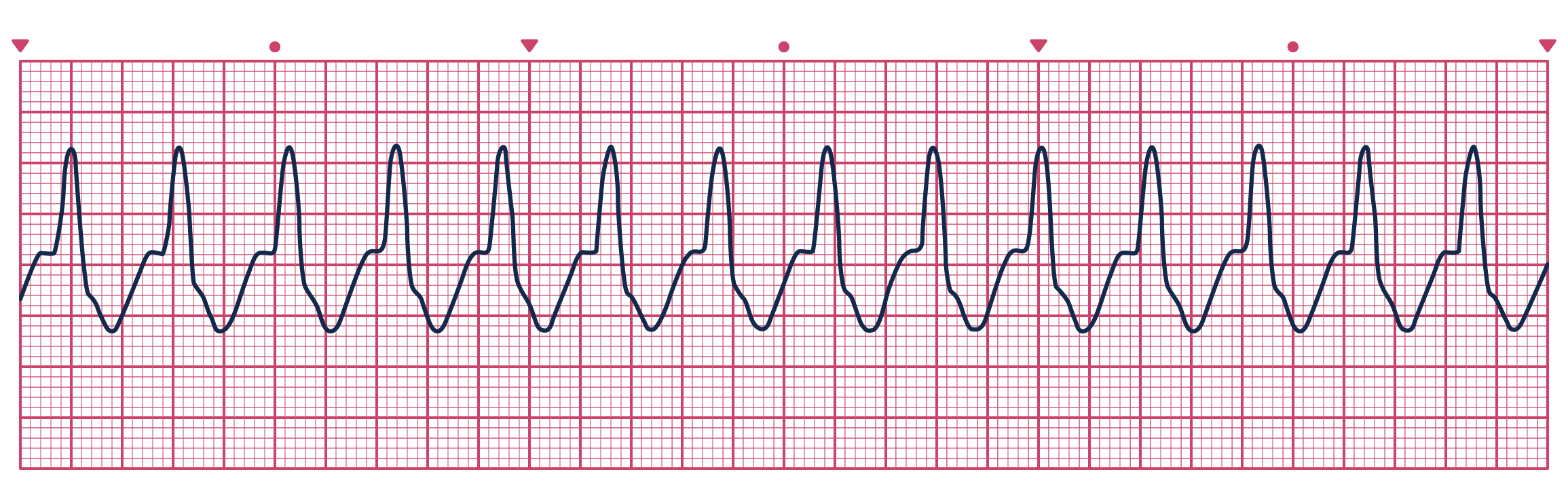
A patient presents to ED with chest pain and this trace. What would you do?
Interpretation management
Allows detention of a patient with a mental health disorder who is at risk of harm to themselves or others (nothing to do with capacity)
Note:
| Section 2* | 28 days for assessment and treatment (by 2 doctors but one must be MHA approved) |
| Section 3* | 6 months for treatment (by 2 doctors but one must be MHA approved) |
| Section 4 | 72 hours for emergency assessment (by 1 doctor, and an approved mental health practitioner, or the patient’s closest relative) |
| Section 5(2) | 72 hours detainment for assessment of patient already in hospital (by doctor in charge of patient’s care) |
| Section 5(4) | 6 hours detainment for assessment of patient already in hospital (by approved mental health nurse) |
NB: common law may be used in emergencies when there is no opportunity to determine a patient’s mental capacity or mental state. It may be used for detention if the patient is at risk to themselves or others; and/or for the minimum treatment of any illness if urgent intervention is required to save the patient’s life or to prevent a significant deterioration in their condition. It is used most frequently in the emergency department.
You are called to a patient on the medical unit admitted with a paracetamol overdose. They have a history of depression and have been assessed as high risk. They are trying to leave and the nurse asks you what to do?
Oops! This section is restricted to members. Click here to signup!
A patient who is currently sectioned under section 3 in a mental health unit with schizophrenia, develops an acute limb ischaemia. They are presented with the risks of death without amputation. They decline the operation. What would you do?
Oops! This section is restricted to members. Click here to signup!
A patient who has encephalitis needs treatment with IV aciclovir. They remove their cannula and refuse for another one to be reinserted. They are unable to understand the risks of not having the treatment. What do you do? What if they repeatedly pull it out?
Oops! This section is restricted to members. Click here to signup!
An 82 year old female is brought to the emergency department after ingesting organophosphate. She will not survive without treatment. She does not have a history of a mental health disorder. She understands, retains, weighs up and communicates the decision to not have treatment. She does not seem depressed. She explains she has nothing to live for anymore as her husband died 5 years ago, she has no friends and wants to die. What do you do?
Oops! This section is restricted to members. Click here to signup!
Want to find out how 99% of people passed their exams?